Miscellaneous
8 Useful Tips to Improve a Nurse Charting Cheat Sheet
Published
3 years agoon
By
admin
Registered nurses value charting cheat sheets and use them as a go-to tool in exercising best practices for nursing documentation. Recording in maintaining the details of patient care, welfare, and recovery, nursing cheat sheets aid with thorough examples of sequential steps to be followed.
Initially, nurses may not feel it is crucial as there is very little stress given in most programs about the importance of documentation and compliance requirements to follow when recording patient details.
However, when a specific ailment is encountered for the first time then it helps the nurse through the patient’s care. For instance, a completely new patient may not realize the importance of hydration in severe diarrhea, but with a reference to the nursing electrolytes cheat sheet, one can easily assist the patient back to recovery.
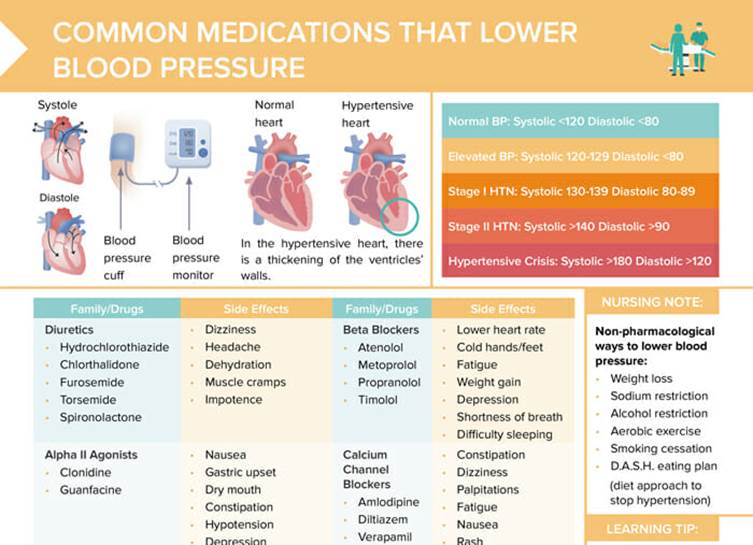
Need for proper nursing charts and cheat sheets
-
High-ticket demand
Nurses deal with numerous patients, and the nursing documentation needs to rise with every new admission. There is a huge amount of patient data to be updated and maintained regularly. Most nurses take several years to develop a nursing cheat sheet of their own that works like a well-oiled machine.
-
Inadequate training
Some schools do not prepare nurses enough with nurse charting and patient documentation training, which is problematic specifically for new nurses on the job who frequently struggle with tasks.
-
Accurate record maintenance
Nursing documentation offers precise data on each medical treatment given to a patient. Healthcare facilities need to comply with sufficient paperwork to prove that the right care was given as per the regulations and laws of the land. In case of an official complaint by a patient, nursing documentation is a handy tool for all the key information detailing the treatment course during a nurse’s shift.
-
Quick reference for care providers
The doctors who are seeing the patient after an interval can refer back to the documentation to see the progress of the recovery. It provides essential clinical information to the care providers enabling them to make accurate choices for patient safety. Without documentation, it is not possible to access the right patient data or have any inkling about the treatments already administered to the patient.
After understanding the importance of nursing documentation, if you are looking for tips to maintain nursing charting cheat sheets, check here:
1.Follow HIPPA compliance
One important point of HIPPA compliance is the safety and integrity of patient data. So ensure that you don’t randomly write patients’ names and or their details in the notes. At the end of the shift, after you have recorded the information in the treatment plan, remember to shred your notes.
2.Prioritize documentation
Even on a busy day, it is recommended that a nurse does not push the documentation till the end of the shift. One tends to forget what was done at the start of the shift and may not record trivial information that will prove to be critical at a later stage and may result in gross negligence on clinical grounds. Senior nurses always follow the rule to document on the fly. It is as important as moving on to the next patient in line.
3Legible and grammatically correct
It is important to document for future reference by some other nurse or doctor. So it is important to write your notes in legible handwriting, a readable language without any slang or short words, or grammatical mistakes.
4.Use Digital tools
Several templates and tools can aid in nursing documentation as per the charting and cheat sheets. You can use these tools to record the information. The advantage of using automated software to record data eliminates spelling and grammar mistakes. If you use charting software, you can turn on the notifications for any important changes in the patient’s data that will be useful for care delivery.
5.Chart in real-time
It is a bad idea to chart in advance as one may need to strike out information that will still be available for the record. So, it reflects upon the nurse as a bad practice of her workflow for documentation. Even late entering and corrections should be avoided and charting has to be finished at least for important aspects in real-time. One can use tabs to record all the information in a template in current times of technology.
6.Objective points
Any charting notes have to specify the facts objectively. It should never record the opinion of the nurse. Nurses can use these notes at a later stage for the learning curve, but the documentation as such should be free of any influential matter from the nurses’ side.
7.Within normal limits
Understandably, a few days are crazy in terms of the number of patients that warrant a nurse’s attention. On such days also it is important to record the information that is WNL or within normal limits. Once the nurse has some space and time in her schedule, they can finish the report.
8.Forward-thinking
Only a nurse can understand what it is like being one. So if you come into a shift and find all the patients’ charts are haphazard or incomplete, you have a lot on your plate for the day. Likewise, if you don’t write down the details meticulously for the next nurse to comprehend, then it will be difficult for the next shift nurse who will replace you.
It is also important to note details like patient education and family interaction in the course of your shift.
Conclusion:
Healthcare institutions must follow standards for nursing paperwork for regulatory compliance with federal and state laws. It is necessary to record either in nursing software or alternative approved methods to record documentation relating to patient care and nursing assessments.
Any new treatments and drugs used in the course must be entered into the patient’s clinical records. This step is necessary to provide a base for the caregiver in charge to look into a patient’s history and medical background and avoid medical malpractice or negligence. So, it pays for budding nurses to do their groundwork and take training for documenting correctly using charting and cheat sheets.
You may like
Miscellaneous
What Makes Jet Skis Different From Waverunners?
Published
2 months agoon
April 3, 2026By
David Smith
PWCs provide a way of cruising forward in style in addition to being fun to operate. They can be rented or purchased in different types. Among the most popular types are wave runners and jet skis. While these two boating options both offer thrilling adventures, they differ in a few important ways. Our goal is to help you determine which one best fits your needs so you can make an informed decision.
Factors Differentiating You
A PWC or water scooter includes a WaveRunner and PWC. There are some select differences between two types of watercraft, but both are under the same brand. These watercraft are part of the same family, but they perform different functions. Below are some ways they differ:
- During driving, sitting or standing is more comfortable
- Storage space is available
- Severity
- Reliability and speed
Jet Skis: What Are Their Purposes?
In 1973, Kawasaki designed the jet ski as a version of the personal watercraft. Several personal watercraft have become synonymous with the term “Jet Ski” due to its immense popularity. Jet skis and WaveRunners, on the other hand, differ in several ways.
Stand-up PWCs were the only ones available in the early days. They were well-known for their high performance. The machines have sometimes been compared to motorcycles on water. If you want a PWC that can combine speed and trickery, then Kawasakis are a great choice. Compared to WaveRunners, these boats are generally more expensive because of their extraordinary performance.
Waverunner: What Are Its Purposes?
Yamaha made its foray into personal watercrafts in the late 1980s. When they introduced their first sit-down watercraft, the market was completely changed. The WaveRunner can carry one to two people, so even those with knee injuries can access the PWC.
Families can take advantage of the family-friendly relaxation potential that WaveRunners for sale provide. They are seen as one of the most popular options among PWCs. In addition, Yamaha offers stand-up jet skis called SuperJet.
How Should I Proceed?
Kawasaki jet skis and Yamaha WaveRunners have both been rated as the top personal watercrafts. In addition to standing and seated seating options, both brands offer multi-person seating as well. Your needs and personal preferences go a long way in helping you choose the right watercraft.
The following breakdown can help you determine which PWC is right for you:
Jet skiing has several advantages
You might want to try a jet ski for sale if you are looking for the fastest, most powerful ride. Kawasaki is renowned for its quality design and craftsmanship when it comes to personal watercraft. Choosing a jet ski is typically an extreme sports enthusiast’s choice because of its powerful engine. Even so, it is important to remember that all this high-end technology comes at a price.
Also, keep these things in mind:
- Protective seat covers
- This speaker
- SLO (Smart Learning)
The benefits of waverunners
In terms of cost-efficiency and family-friendliness, WaveRunners are an excellent choice. Controls on this jet ski are easier to use than those on Kawasaki’s jet ski.
A feature like this is useful for beginners who are hesitant to go too fast. The WaveRunner can also be more easily maintained. The technology on Yamaha WaveRunners is typically less sophisticated than that of Kawasaki, so they are usually easier to repair.
The following points should also be considered:
Ensures safety by providing * safety features
- Fuel capacity is greater
- A rudder assists with steering
If You Want To Try Jet Skiing, Marco Island Is The Place To Go
The 10,000 Islands area is full of fun activities for everyone to enjoy while visiting Marco Island Jet Ski Tours and Rentals. Join us for one of our top-tier jet ski tours to explore the stunning beauty of the area.
What Jet Skis Are All About
It is quite a simple machine, the jet ski. One of the most important parts of the jet ski is its wheel, which pulls on the ground underneath it in order to move.
Powered by motors that draw water in and push it out, jet skis move through the water. By the water being drawn in, the jet ski is propelled forward, but its power is generating the forward movement. Once you’ve collided with some water surrounding you, you begin moving.
The analogy of swimming can be used. As you paddle your hands and feet through the water, you change your position by pushing the water behind you. You use your medium to pull and push with you whenever you move, just like when you are driving or climbing a mountain.
Water can get into the engine of a jet ski, but how?
Water enters the engine impellers on jet skis. The water enters the vessel via the impeller, which is a motorized fan. Jet ski impellers are designed to remove air, while normal fans are designed to move air. Water is continuously drawn into the ski by the jet impeller and pushed out by the jet propeller.
As soon as the water enters the watercraft, the jet propulsion system expels it. A stream of propelled water propels you forward as it moves between you and the surrounding water.
Since air is significantly lighter than water, a jet ski filled with water won’t budge when lifted out of the water. The water would simply fall to the ground, so you would not be able to move forward.
Miscellaneous
Everything You Need to know about Capital Gains
Published
2 months agoon
April 2, 2026By
admin
What Exactly Is a Capital Gain?
A capital gain is the increase in the value of a capital asset when it is sold. A capital gain occurs when you sell an asset for more than you paid for it. Almost any asset you own is a capital asset, whether it’s an investment (such as a stock, bond, or real estate) or something you bought for personal use (like furniture or a boat). When you sell an asset, you realise capital gains by deducting the original purchase price from the sale price. In certain circumstances, the Internal Revenue Service (IRS) taxes individuals on capital gains. Read more about capital gains tax india here.
Understanding Gains on Capital
As previously stated, capital gains are the increase in the value of an asset. These profits are typically realised when the asset is sold. Because of their inherent price volatility, capital gains are commonly associated with investments such as stocks and funds. They can, however, be realised on any security or possession sold for a price greater than the original purchase price, such as a home, furniture, or a vehicle.
Capital gains are classified into two types:
Those who make short-term capital gains are those who own something for less than a year and then sell it.
- Long-term capital gains are made when an asset is sold after more than a year.
- Short-term and long-term gains must both be reported on your annual tax return.
Understanding and incorporating this distinction into an investment strategy is especially important for day traders and others who take advantage of the increased ease of trading in the market online.
Mutual Funds and Capital Gains
Mutual funds that accumulate realised capital gains during the tax year are required to distribute them to shareholders. Many mutual funds distribute capital gains just before the calendar year ends.
Shareholders receive the fund’s capital gains distribution and a 1099-DIV form detailing the amount and type of gain (short-or long-term). When a mutual fund distributes a capital gain or dividend, the net asset value (NAV) decreases by the amount of the distribution. A capital gain distribution has no effect on the total return of the fund.
Capital Gains Exemplification
Here’s a fictitious example to demonstrate how capital gains work and how they’re taxed. Assume that Jeff paid $350 per share for 100 shares of Amazon (AMZN) stock on January 30, 2016. He then decided to sell all of the shares on January 30, 2018, for $833 each. Assuming no fees were associated with the sale, Jeff realised a capital gain of $48,300 ($833 x 100–$350 x 100 = $48,300).
Jeff makes $80,000 per year, putting him in the huge income bracket ($40,001 to $441,500 for individuals and $80,001 to $496,600 for those married filing jointly) that qualifies for a 15% long-term capital gains tax rate.
As a result, Jeff must pay $7,245 in tax on this transaction ($48,300 x 0.15 = $7,245). Find more details about income tax slab rates here.
Miscellaneous
How to Simplify Your Inventory Management System by Using Barcodes and QR Labels
Published
2 months agoon
April 1, 2026By
admin
Keeping track of every product can be difficult and time-consuming. Using QR labels and barcodes is an easy way to streamline your inventory management system and keep track of your stock’s origin, destination, quantity, and delivery time frame.
This simple method will allow you to have a more accurate record of your company’s inventories and make it easier for you to monitor any changes during transit. In addition, these labels are entirely customizable.
You can add specific information about each product so that all relevant parties know what needs to happen when each item arrives at its final destination. Here are some tips on simplifying your inventory management system with barcodes and QR labels.
What Are Barcodes and QR Labels?
Barcodes are a type of machine-readable code that barcode readers can scan. QR (Quick Response) labels are a way to put an easily scannable barcode on just about anything. They provide information or links to websites or social media pages.
You can also use them for your barcode inventory management. You can create your QR labels using free online tools, which allow you to add a link and text of your choice.
Barcodes and QR labels are often used in retail stores to quickly and accurately track inventory. Still, you can also use them for many other purposes, such as tracking shipments or organizing library books.
Identify Industry Standards
There are various barcode standards that industry groups have created. Which type you use depends on your needs, but when designing a new barcode inventory system, it’s essential to consider which industry standards your inventory will adhere to.
You’ll also want to make sure that your equipment can read all of these barcodes. Industry-specific barcodes include Code 39 used for the automotive industry and the ITF-14 used by retailers, manufacturers, and distributors.
If you’re unsure which industry-standard suits you, ask a few people in your industry what they use or look at what other companies in your area use.
Choose a Scanner
Select a scanner to automate your inventory management system. This allows you to scan, track, and maintain all of your products without manually writing down each product’s details.
Some simple scanners that might work for smaller businesses include a wand, handset, or desktop models. Each scanner has its pros and cons, so choose one that works best for your needs and budget. Do some research on which features are most important to you before purchasing one.
Build a Master List of Inventory Items
Creating a master list of inventory items is a great way to simplify your inventory management system. You can create a master list by scanning or typing each item into a spreadsheet if you’re currently using a paper-based system.
A suitable method is to create multiple lists for different kinds of products. List everything from office supplies to furniture and organize each category by item number. Note the quantity on hand, purchase price, expiration date, and other relevant information.
Be sure to create separate lists for items that are seasonal, discontinued, or sold out altogether. You can take these factors into account when making purchasing decisions in the future.
Implement Changes With Software
Businesses with multiple locations should also consider automating their barcode inventory system. With software, you can keep track of your physical inventory. Use a spreadsheet or inventory management program to keep track of your entire product line.
Barcodes and QR labels are great ways to ensure that your inventory is continually updated and accurate. You can scan codes on products that come into your store and barcodes on products that leave your store. This will help you better manage your inventory.
Create Barcodes
Wondering how to create barcodes for inventory systems? Before you can start using your inventory management system, you’ll need to assign a unique identification number to each product. Decide on what labeling information you want to give to each barcode (e.g., product name, brand name, product category, purchase cost).
You’ll also need to choose an appropriate type of barcode based on how much information you plan to include in it. Once you have selected a label size and type of barcode, print out several samples of barcodes with different kinds of labels.
Stick them onto products similar to those you will be selling and see if they can work properly at various distances, lighting conditions, etc. If there are problems with any labels or scanners after testing them for several days, change your choices accordingly until everything works perfectly before printing thousands of labels.
Wrap Up
Barcodes and QR labels are extremely useful in simplifying inventory management. You can place these labels on any product to provide a quick way to track inventory.
The technology used for barcodes and QR codes is constantly evolving, making it easier to use these devices in your business.

Explore New Dimensions of Advertising with Custom Poster For Marketing Campaigns

Level Up Your Business with Vinyl Banners

What Makes Jet Skis Different From Waverunners?

Best Ways to Earn Money Online Using Tech Skills in 2026 (Step-by-Step Guide)

What is Web3 Technology? Simple Beginner-Friendly Guide to the Decentralized Web

How to Choose the Right Antivirus Software For PC in 2026: Complete Guide

Beginner’s Guide to Generative AI in 2026: Everything You Need to Get Started

Everything You Need to know about Capital Gains

Do You Often Get Bored And Have Nothing To Do? Try Playing 13 Rummy Card Games, It Has A Lot Of Benefits

How to Simplify Your Inventory Management System by Using Barcodes and QR Labels
Trending
-

 Gaming2 months ago
Gaming2 months agoIoT and Gaming – A World of Unlimited Possibilities!
-

 Tech2 years ago
Tech2 years agoThe Evolution of Mobile Technology: Past, Present, and Future
-

 Gaming8 months ago
Gaming8 months agoIs the Forest Cross Platform or Not – Find Out All You Need to Know!!
-

 Gaming6 months ago
Gaming6 months agoIs Europa Universalis 4 Cross Platform Multiplayer?

